|
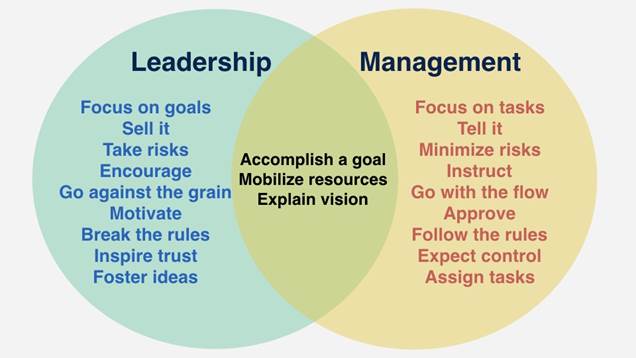
11/16/2018 0 Comments Too much leadership?I’ve experienced first-hand the tremendous rate of unsettling change in the NHS. Within one six month period two reorganisations affected my team. The first one, which happened only six weeks after two of them were appointed, led to both their job descriptions changing and one being moved to another department. Then, just five months later, a formal consultation began for a restructure of the wider team which affected our remit and the reporting structure we worked within. In terms of Tuckman’s theory of team formation (1), it makes it very hard, if not impossible, for a team to move into a stage of high performance with so much in flux. Given how unpopular constant restructuring is (2), the struggle to retain and recruit staff, and high sickness rates due to stress and anxiety, why does this continue? As a curious organisational development (OD) practitioner I did some research and came across a blog (3) indicating Penny Camplings’s research proposing that the constant need for change is a way of managing organisational anxiety that comes from holding patient wellbeing – and often lives – in its hands. That makes sense, because when we’re anxious it’s really hard to sit still and do nothing, but often the activity is a way to displace the nervous energy of the emotion, rather than a productive way of dealing with its cause. To sit with the huge pressures the NHS is under, including the constant public scrutiny and increasing funding and staffing pressures, to acknowledge the discomfort and perhaps listen to what it is telling us might be a more productive, if much harder, strategy. However I think there’s something else afoot, too. Following the King’s Fund report (4) earlier this year, revealing that many Board-level roles last as little as a couple of years, coupled with an established culture of interim appointments and secondments, there is also the pressure to show very quickly in a new role that you can perform as an effective ‘leader’. I use the quotes intentionally, for I believe that this term is often misunderstood. When you google leadership and management, this kind of summary commonly comes up: Management is today often conveyed as being conformist, old-fashioned and static. Now that the field of management development is rapidly being renamed leadership development, if we understand leadership only as it is conveyed above (which contradicts the emerging discourses around compassionate, mindful and distributed leadership), it is imperative for short-term appointees, or those in substantive roles who understand they may only last a few years, to make an impact early on, to challenge existing practice and be seen to transform and change things. So sitting with and listening to the underlying anxiety of staff and teams without doing anything about it is quite likely to be seen as a weakness instead of a strength.
And we all endorse this in many ways. When was the last time you asked someone in a job interview: ‘When did you lead a challenging new project or initiative?’ and not: ‘When did you decide to keep things the same?’. If you don’t expect to stay long in a role, you’re going to want to instigate change as quickly as you can, so you can talk about the impact you created in your next job interview – because, for sure, that’s what you’ll be asked about. In both the examples from my own story, the change was instigated by individuals appointed on six-month contracts who were acting, or advising, at Director level. Asking around staff who have been working in the NHS system for decades, this is not uncommon. So here is a plea, and a personal commitment, to speak well of the continuing need for good management, and be clear that leadership can mean leading change but also protecting the status quo if and when required. Because only in this way will enough NHS staff maintain the psychological safety to keep themselves well and deliver the patient care we will all, sooner or later, require of them.
0 Comments
Leave a Reply. |
AuthorThis blog shows the range of interests and activities that Kate delights in - and shares her news Archives
June 2022
|
 RSS Feed
RSS Feed
